Information center / Gynecology / Monthly Spotlight / Prevention / Science / VM Med / Women's health
Is It Endometriosis or Period Pain? How to Tell the Difference

(Tina Dawn/ VM Med) — Menstruation, and the pain and discomfort that routinely come with it, are a normal part of a woman’s monthly cycle. In fact, painful periods are so common that there’s even a medical term for them: dysmenorrhea. Painful periods are usually accompanied by menstrual cramps, throbbing, cramping pain in your lower abdomen, as well as other symptoms, such as lower back pain, headaches, nausea, and diarrhea.
Period pain is not the same as premenstrual syndrome (PMS), which often starts one to two weeks before your period starts, and causes additional issues.
What is Endometriosis
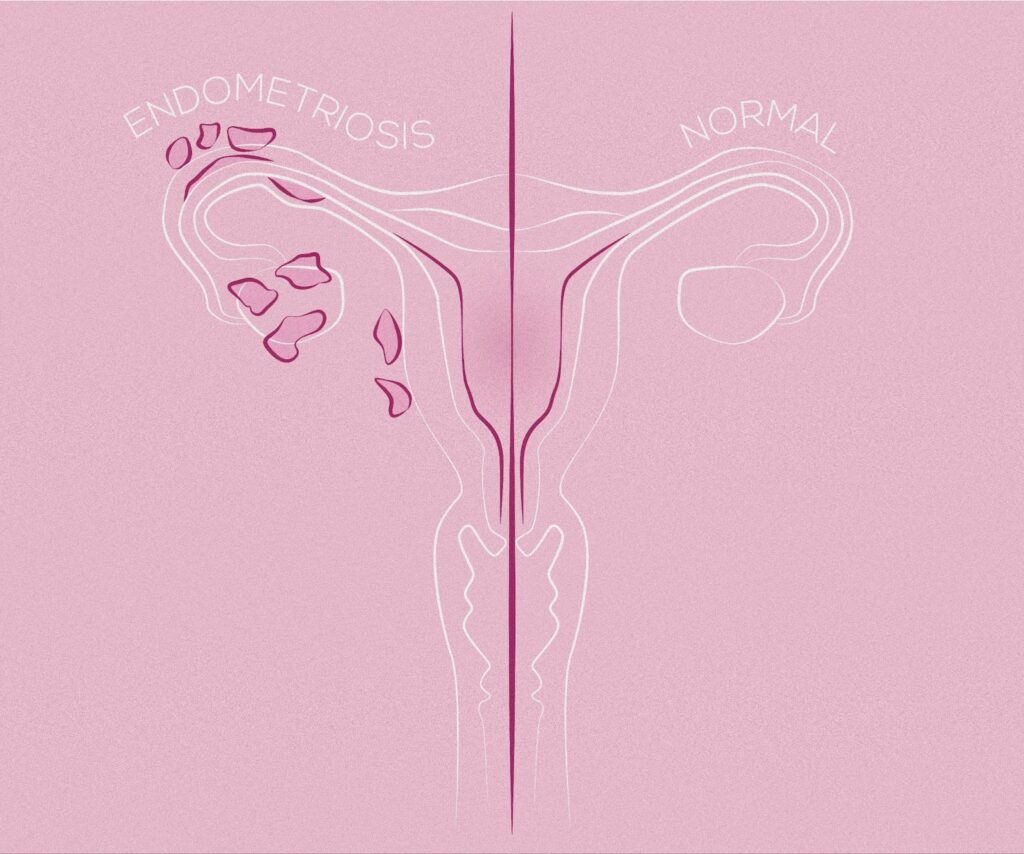
Endometriosis, on the other hand, is an inflammatory disease where endometrial-like tissue grows outside of the uterus, causing chronic pelvic pain, painful periods, painful sexual intercourse, bowel and bladder symptoms, and infertility. It’s most often found on the ovaries, fallopian tubes, and in the gastrointestinal tract.
Given that most women experience some degree of period pain, it’s often easy to minimize or dismiss painful signs of endometriosis as normal period cramps, which can prevent them from receiving proper diagnosis and treatment.
Considering endometriosis affects around 10 percent of women of reproductive age and can even cause infertility, it’s important for women to be able to understand and distinguish the difference between the pain of their monthly menstrual cycle and a chronic disease.
Adenomyosis vs Endometriosis
While both adenomyosis and endometriosis are painful progressive disorders involving endometrial tissue, they are distinct conditions located in different locations of the body and should be understood as separate. In some cases, women may suffer from both disorders.
The main difference: In adenomyosis, cells grow inside the muscular wall of the uterus, causing the inside of your womb to get thicker and bigger. Endometriosis, on the other hand, occurs outside the uterus (the ovaries, for example).
Common Symptoms of Endometriosis
According to John Hopkins Medicine, there are five common symptoms of endometriosis, which is also commonly known as endo.
Common symptoms of endometriosis:
• Severe pelvic pain
• Painful intercourse
• Painful periods
• Heavy menstrual bleeding
• Pain with urination and/or bowel movements
• Infertility
While these signs may be very common among women suffering from endometriosis, that doesn’t mean that if you’re experiencing some of these, you’re definitely dealing with the chronic illness. That’s why a proper diagnosis by a medical professional is important.
Common Symptoms of Adenomyosis
• Painful and heavy menstruation
• Chronic pelvic pain
• Painful intercourse
• Enlarged uterus
• Infertility

Endometriosis vs Polycystic Ovary Syndrome (PCOS)
Although both endometriosis and PCOS are hormonal disorders, the former is caused by excess androgens (male hormones), affecting ovulation. This causes missed periods, excess hair growth, acne, weight gain, hair loss, and insulin resistance. Endometriosis is tissue growth causing inflammation and severe pain. Both endometriosis and PCOS cause menstrual problems, which can lead to heavy bleeding.
Even though severe pain and irregular periods are symptoms of both conditions, endometriosis and PCOS are not the same. It’s important to monitor your periods and pain levels to start understanding what you might have. For example, while pain may be a symptom of both, if you’re also dealing with excessive hair on your chest and face, it’s very likely to be PCOS. The only way to be certain is a proper PCOS diagnosis through a pelvic exam, ultrasound, and blood work.
Stage 4 Endometriosis
The severity of endometriosis can vary among individuals and, in some cases, it can be a progressive condition. In some cases it remains stable. Endometriosis is usually classified into four stages or categories, ranging from Stage 1, which is accompanied by minimal symptoms and pain, to stages 2 and 3, accompanied by mild and moderate pain, to Stage 4, usually accompanied by severe pain, widespread scar tissue, large ovarian cysts, and an increased risk of infertility.
While stage 4 endo can often be associated with reduced fertility and difficulties conceiving, many people living with stage 4 endometriosis can still successfully fall pregnant. Once again, proper diagnosis and treatment is primordial.
Endometriosis Diet

Patients suffering from endometriosis are often offered surgery or medication as a way to manage chronic pain. But a recent medical study found that a change in one’s diet could also help reduce symptoms.
Researchers found that cutting down on things like dairy, gluten, caffeine and alcohol could improve endometriosis symptoms. Drinking less alcohol improved pain in 53 percent of women. Eating less gluten improved it by 45 percent, consuming less dairy reduced it by 45 percent and cutting down on caffeine reduced pain by 43 percent.
Other dietary changes that offered improvements in pain reduction were eating less processed sugar, less processed food, and taking supplements like turmeric and magnesium. While more research needs to be done, doctors speculate that the anti-inflammatory properties in these dietary changes help decrease inflammation in the body, since there’s an inflammatory component to endometriosis.
Why Proper Diagnosis and Treatment are Important

Because of how complex and varied symptoms can be, as well as how endometriosis often mimics other gynecological conditions, it requires the specialized care of a gynecology centre and doctors that can both properly diagnose and treat the condition.
A laparoscopy—surgery where a doctor inserts a tiny video camera into the patient’s abdomen to look for evidence of scarring or cysts—is the only way to confirm someone has endometriosis.
There is no current cure for endometriosis, but an early diagnosis can help a person receive timely treatment, which may help improve their overall outlook. Since there’s no such thing as a one-size-fits-all approach to women’s health, individualized treatments and tailor-made management strategies can help patients manage symptoms and improve their quality of life.
VM Med Gynecology Centre
At the VM Med Gynecology Center, we are committed to supporting every aspect of women’s health throughout life’s stages. In a welcoming and compassionate environment, our team provides specialized counselling and treatments for a wide range of concerns—including menstruation, menopause, hormonal imbalances, sexually transmitted infections, and both benign and malignant gynecological conditions.
During your consultation, your physician will take the time to listen to your concerns, perform any necessary examinations, and recommend additional services when appropriate. Our centre offers comprehensive care, from annual exams and cervical screening to contraception, family planning, and menopause management. We also provide specialized clinics for conditions such as vulvodynia, vaginismus, and vulvar skin disorders, as well as advanced procedures including colposcopy, hysteroscopy, minimally invasive surgeries, and innovative treatments like MonaLisa Touch and platelet-rich plasma therapy.
The Expertise of Dr. Lorraine Dontigny
Dr. Lorraine Dontigny (M.D., F.R.C.S. (C) is an Obstetrician-Gynecologist at VM Med. Her expertise lies in general gynecology, with a special focus on genitourinary syndrome in postmenopausal women. She completed her medical training and residency at l’Université de Montréal. From 2000 until 2022, Dr. Dontigny was a valuable member of the LaSalle Hospital’s obstetrics and gynecology team in Montreal, and an assistant professor at McGill University and l’Université de Montréal. Dr. Dontigny performs a number of procedures, including colposcopy, hysterosonography as well as the unique MonaLisa Fractional CO2 Laser Therapy.
Additional Resources
For more information, you can read our extensive archive of VM Med blogs, including Why Annual Checkups Matter: The Power of Preventive Care or How The Thyroid Impacts Women, Hormones, and Menstruation.
Still have questions? Book a consultation with our experts. We support every aspect of our patients’ health throughout the course of their lives.
Categories
